The Family Initiative has been tracking and reporting on research on fathers in neonatal care since 2015 on FamilyIncluded.com. It became apparent that some interesting and new ideas were emerging in newly published articles. In response to this, the Family Initiative approached all the authors and proposed a joint effort to report on all the new evidence.
We have since published an article in the Journal of Neonatal Nursing - Fathers in neonatal units: Improving infant health by supporting the baby-father bond and mother-father co-parenting.
This discusses the findings from 50 pieces of research in recent years on fathers in neonatal units.
The principle finding is that understanding and supporting father-infant attachment and supporting co-parenting improves the health of the baby and helps both parents to care for the baby and for each other.
RESEARCH REVIEW
NEONATAL DADS
INTERNATIONAL WORKING GROUP
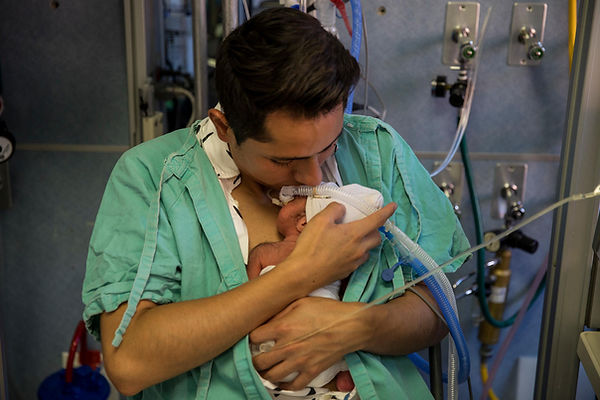
The Family Initiative has convened the International Neonatal Fathers Working Group, involving 11 researchers and practitioners who have championed better engagement and support for fathers whose infants are being cared for in neonatal units.
Our members are:
-
Esther A. Adama, Edith Cowan University School of Nursing and Midwifery, Perth, Australia
-
Nancy Feeley, Ingram School of Nursing, McGill University; Centre for Nursing Research & Lady Davis Institute - Jewish General Hospital, Montréal, Canada
-
Duncan Fisher, The Family Initiative, UK [Project Lead]
-
Craig F. Garfield, Departments of Pediatrics and Medical Social Sciences, Northwestern University Feinberg School of Medicine; Lurie Children's Hospital of Chicago, USA
-
Jillian Ireland, Poole Hospital NHS Foundation Trust & Visiting Faculty Bournemouth University, UK
-
Minesh Khashu, Poole Hospital NHS Foundation Trust Poole & Bournemouth University, UK [Research Chair]
-
Flora Koliouli, Laboratoire Interdisciplinaire Solidarités, Sociétés, Territoires (LISST), University of Toulouse, France
-
Birgitta Lindberg, Department of Health Sciences, Luleå University of Technology, Sweden
-
Betty Nørgaard, Department of Paediatrics, Lillebaelt Hospital, Kolding, Denmark
-
Livio Provenzi, Scientific Institute IRCCS Eugenio Medea, Bosisio Parini, Italy
-
Frances Thomson-Salo, Centre for Women's Mental Health, Royal Women's Hospital, Carlton, Australia
-
Edwin van Teijlingen, Centre for Midwifery, Maternal & Perinatal Health, Bournemouth University, UK
RESEARCH REVIEW
The Family Initiative has been tracking and reporting on research on fathers in neonatal care since 2015 on FamilyIncluded.com. It became apparent that some interesting and new ideas were emerging in newly published articles. In response to this, the Family Initiative approached all the authors and proposed a joint effort to report on all the new evidence.
We have since published an article in the Journal of Neonatal Nursing - Fathers in neonatal units: Improving infant health by supporting the baby-father bond and mother-father co-parenting.
This discusses the findings from 50 pieces of research in recent years on fathers in neonatal units.
The principle finding is that understanding and supporting father-infant attachment and supporting co-parenting improves the health of the baby and helps both parents to care for the baby and for each other.
WHAT NEONATAL FATHERS SAY
These are quotations from the published research that we reviewed.
“I did a bit of kangaroo with him and when I looked at him….wow! I’m going to be paternal, I know.”
“When I first saw M., it was magic, a miracle! I was all alone in the bloc.”
“The first time I held him skin-to-skin, it was really, like, wow! It was like a communion.”
“I looked at my son and then my daughter and then my wife and I just felt, damn I’m so happy.”
“I have never been this stressed before….I take care of the other children at home and of my job, but I also need to be here – I want to be here as well.”
“As a father, you feel left out.”
"I don’t want to be weak in front of my wife. I don’t think she knows how bad I am hurting right now."
“I have to cheer her up, but no one helps me. It is difficult to bear. I do not show that I am burnt out; instead, I suppress my feelings.”
“I wouldn’t want my wife asking me how I feel.”
“Everybody around the situation is focused on mom/baby. Dads are left to worry about everything and everyone. As a dad, you may feel lonely.”
“It would have been helpful to have maybe more contact with NICU fathers such as men with children who were either currently or had been in the NICU at some point.”
RECOMMENDATIONS FOR PRACTICE
We make three key recommendations to improve infant health on the basis of the evidence:
-
Support the father-baby bond in the same way the mother-baby bond is supported.
-
Pay attention to the differences between mothers and fathers, both within individual families and also in relation to different gendered social expectations experienced by each.
-
Support team parenting, or co-parenting, between the mother and father.
We also make 12 practical recommendations for practice:
-
Assess the needs of mother and father individually.
-
Consider individual needs and wants in family care plans.
-
Ensure complete flexibility of access for fathers to the neonatal unit.
-
Gear parenting education towards co-parenting.
-
Actively promote father-baby bonding, particularly skin-to-skin, even in the presence of the mother.
-
Be attentive to fathers hiding their stress from both professionals and their partners.
-
Inform fathers directly not just via the mother.
-
Facilitate peer-to-peer communication for fathers.
-
Differentiate and analyse by gender in service evaluations.
-
Train staff to work with fathers and to support co-parenting.
-
Develop a father-friendly audit tool for neonatal units.
-
Organise an international consultation to update guidelines for neonatal care, including those of UNICEF.
GENDER DIFFERENCES
The research identifies three ways in which fathers start from a different place from mothers:
-
Fathers are often not considered “natural” carers like mothers are, a view that is strongly challenged by biological, neurobiological and psychological evidence.
-
Fathers are often expected to continue working and to look after older siblings.
-
Fathers are under strong social pressure to appear strong and to hide their distress.
Father-baby contact, particularly skin-to-skin, stimulates strong hormonal changes in men – more oxytocin, more prolactin, less testosterone. All these are linked to caring activity (as in mothers). Neurobiological changes also take place triggering ‘emotional empathy’ and ‘socio-cognitive’ networks in the father’s brain (as in the mother’s).
When these two networks are strongly activated, the baby is likely to have stronger emotion regulation and social skills four years later.
